Ben OConnor, BSN
\
Nov 2, 2025
Contrary to popular belief, cardiac rhythm identification isn’t hard. What most of us need is access to a good tutorial and lots of practice. Clinical rotations provide an excellent opportunity to get in there and look at some rhythm strips.
Understanding the most common rhythms is essential for today’s nurse who sees sicker patients. It is also the backbone of advanced cardiovascular life support training, which is a must-have for nurses interested in critical care.
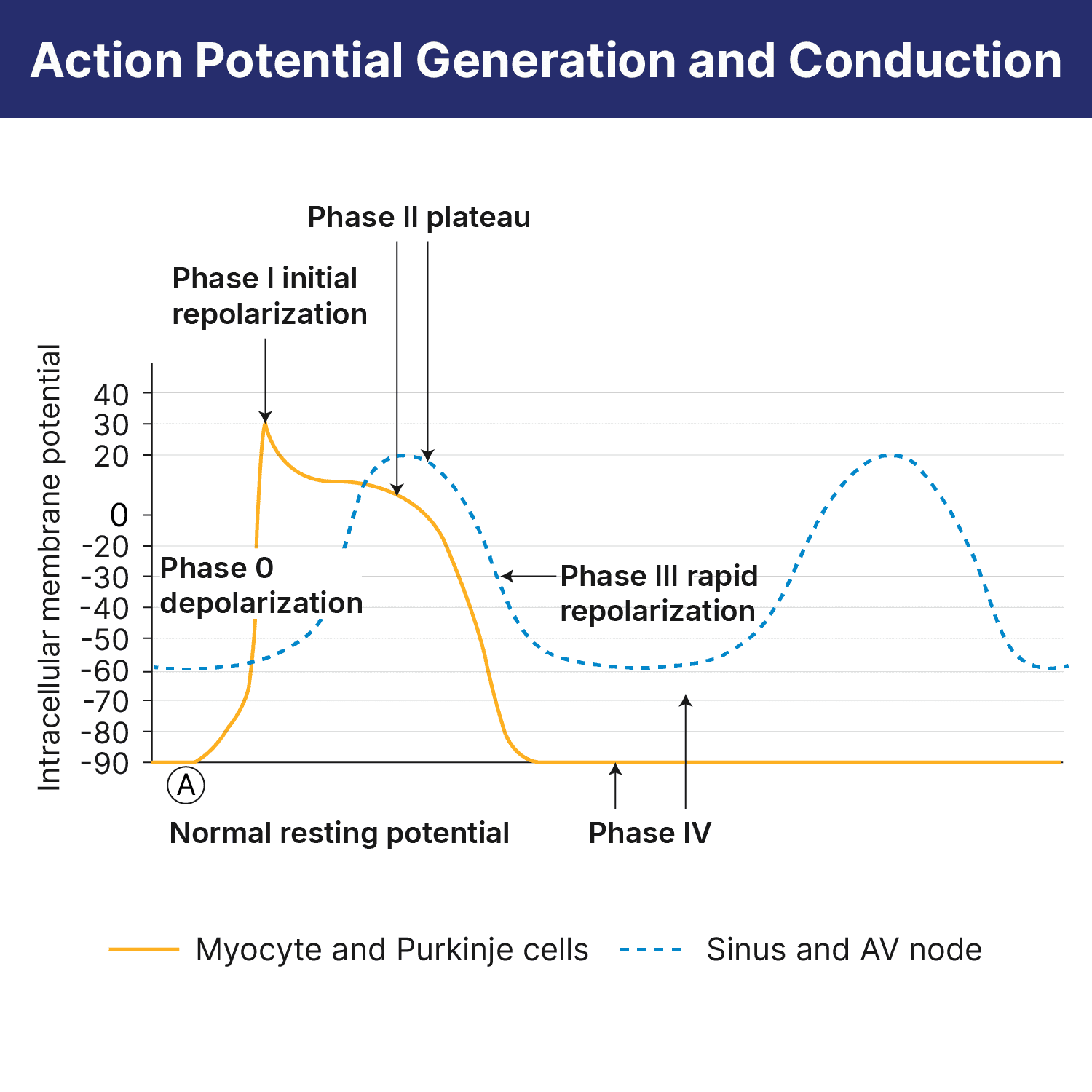
What the ECG Represents
The ECG represents the electrical activity that occurs inside the myocardium (the heart muscle). Demystifying rhythms begins with an understanding of the basic PQRST waveform, which is a graphic representation of the “LUB-DUB” cycle. Some simple rules about each wave tell us what the heart is physically doing. Simply put: Waves in the rhythm represent muscle contraction, and spaces between them (intervals) represent the electrical impulse’s journey through the heart’s conduction pathways.
Normal Heartbeat
For basic rhythm interpretation, we can leave out the Q wave. A Q wave is the first downward deflection leading into the tall QRS complex and is often not seen at all. Analysis of this wave should be left for more experienced providers, so we will ignore it for now.
This leaves us with the following waves:
P wave: atrial depolarization in which the atria contract, producing the “LUB”
PR interval: an impulse traveling from the SA node through the atria and the AV junction to the ventricle
This wave represents the impulse’s journey from the top of the heart through the AV node and down to the Purkinje fibers along the ventricle muscle. It’s important for rhythm analysis, as you will see.
QRS complex: includes the R wave; ventricle depolarization in which the ventricles contract, producing the “DUB”
ST interval: a rest period in which the impulse is over and repolarization begins
T wave: a resting muscle wave
Once we understand what each part of the wave represents, we can apply simple steps to analyze the rhythm.
Hint: The best lead (view) on the monitor to examine is Lead II. Printing a longer strip (rhythm strip) gives the nurse enough QRS’s to assess the rate and the rhythm.
Deconstructing a Rhythm
Look at the rate: Is it fast, normal, or slow?
Calculate the heart rate per minute: In a 6-second strip, the number of QRS complexes multiplied by 10 is the easiest estimate.
Determine the rhythm: Is it regular or irregular? (Measure the distance from each R-R. This distance should be constant.)
Examine the Conduction Pathways
First, determine what the atria are doing. Are there P waves, and are they normal or inverted? The presence of P waves indicates sinus pacemaker origin. Inverted, notched, or misplaced P waves may indicate re-entry mechanisms (that is, current traveling up instead of down), usually from a junctional rhythm or an ectopic source. When you see abnormally shaped P waves or those that are occurring within the QRS complex, it is helpful to seek expert advice.
Then, determine what the ventricles are doing. Check out that large, pointed shape in the ECG zigzag. Is the QRS waveform wide or narrow? Is it normal in shape? If it is wide, conduction is slowed or abnormal. If it is narrow, conduction is normal or too fast.
Last (and most important), determine the relationship between the atria and ventricles. Does each P wave produce a QRS? Is the PR interval constant? Are the P waves farther from the QRS complex than normal? Long PR intervals and dissociated atria and ventricles indicate conduction disturbances (heart block).
One extra step: Look for possible ST-segment elevation. Take note of any obvious QRS abnormalities resulting in elevation of the ST segment. We won’t discuss ST-elevated myocardial infarction (STEMI) or bundle branch diagnoses here, but it’s important to be aware of STEMI when reviewing rhythms. And always have a 12-lead ECG reviewed by a trained provider experienced in complete ECG interpretation. Nurses should be familiar with cardiac assessment (including ECGs), but a clinician is trained to interpret and diagnose the 12-lead reading.


NCLEX Mastery
\
What Happens If You Fail NCLEX? A Smart Retake Plan That Actually Helps
What Happens If You Fail NCLEX? A Smart Retake Plan That Actually Helps
Category

NCLEX Mastery
\
NCLEX Style Questions Explained: What the Exam Is Really Testing
NCLEX Style Questions Explained: What the Exam Is Really Testing
Category


NCLEX Mastery
\
How Hard Is Nursing School?



